Podcast: Play in new window | Download (Duration: 23:16 — 32.0MB)
Subscribe: Apple Podcasts | Spotify | TuneIn | RSS | More
Protective Muscle Guarding
Part Five in the series entitled “Threats to a Proper Knee Replacement Recovery”
This is an educational essay designed to help patients who are facing challenges with their knee rehabilitation at home or in an Outpatient PT setting. We want to acknowledge the valuable contributions of Jason Shepherd, BScPT, Injury Prevention Consultant to this article. To find the other articles on Knee Flexion, Knee Extension, Infection and Deep Vein Thrombosis click here: Threats to a Proper Knee Replacement Recovery.
What is Protective Muscle Guarding?
Dr. Erik Dolton, PhD, has spent considerable time studying the condition known as Protective Muscle Guarding. He says, “when the brain senses bony instability or tissue damage in-and-around the knee joint, information is compiled and ‘fast-tracked’ to the brain where a determination is made as to the degree of threat and appropriate response the situation demands.”
Dr. Dalton continues, “Layering the area with protective muscle guarding is a common decision handed down by the cortex. A protective spasm is the brain’s reflex attempt to prevent further damage to injured tissues. By ‘splinting’ the area with a spasm, muscle ‘locking’ effectively reduces painful joint movements. The brain simply acts to protect the body: ‘When in question, lock the muscle.'” Helping patients avoid PT pain is a major concern of Physio Therapists for knee and other surgeries.

At its most basic level guarding occurs when your therapist pushes your knee one way and you push right back, negating his attempt to help you gain knee flexibility as your body attempts to protect itself.
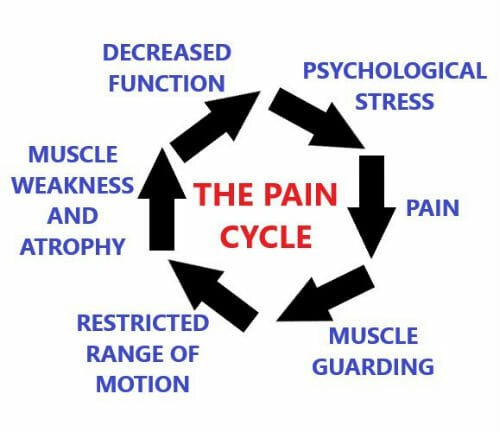
Today’s physical therapist will always be confronted with the mysteries of muscle guarding. And this condition must be dealt with quickly as continued guarding inhibits proper knee rehabilitation. A therapist cannot administer effective therapy if a patient’s protective muscle guarding stops the therapy dead in its tracks. And oftentimes, in addition to the brain’s instinctive reflexogenic response to incoming potentially painful movement, there is the natural reaction to consciously protect oneself from danger. Getting past muscle guarding can be the difference between success and failure (and some unpleasant consequences) for your rehabilitation. For more on guarding and “the pain cycle” see the graphic from Nova Active Rehab, and click here.
Another View on Protective Muscle Guarding (a.k.a. Protective Muscle Spasm)
Notes from Cathedral Chiropractic
Muscle guarding is part of our wonderfully effective self protection mechanisms. However if left untreated it may stop being part of the solution and become part of the problem. As humans we have evolved very effective forms of protection both from injury and from further injury.
- We protect ourselves from injury by having very fast reflexes. When we talk about reflexes we’re not simply talking about what happens when we hit your knee with a reflex hammer, more about your body’s ability to correct an unexpected action. For example stepping off an unexpected curb could result in a nasty ankle sprain if your reflexes are unable to react sharply to prevent a fall. What happens is the stretch receptors in your muscles, tendons and ligaments sense the sharp change in length as your ankle starts to go over. They send a quick warning to the spine. Which sends quick instructions back to the muscles around the joint telling them to contract and prevent a fall. In the mean time a very slow message is sent to the brain letting it know what is going on. Normally it has all happened and over with by the time your brain even knows what is going on.
- We protect ourselves from further injury in a slightly more complex way in acute (happened very recently) injury cases and post knee surgery. Firstly, your sensory nerves send off a huge amount of warnings up the spinal cord to the brain. The joint position sensors (proprioceptors), stretch receptors and pressure receptors have a field day giving your brain over enthusiastic information about the stress that the injured part is experiencing. The brain has to make sense of all of this sensory information and invariably will decide to plonk it all into one category and call it pain. Next the body mounts and inflammatory response which not only works to resolve the injury but also prevents further injury by giving you a healthy dose of pain. Pain is a great inhibitor to movement so while all of this is going on you will most likely move the injured part as little as possible which is great as it allows your body to get on with the important job of healing itself. Inflammation also causes swelling which has the effect of restricting the movement of the area – great news!
The Consequences of Protective Muscle Guarding
- A common consequence of muscle guarding is muscle fatigue, not only of the muscle in question but those supporting and opposing muscles forced to compensate for the muscle being guarded.
- Another possible repercussion of muscle guarding is the inappropriate and potentially harmful hair-trigger firing of some of the body’s reflexes. The irony about muscle guarding is that the innate intelligence of the body has the muscles in question “believing” that they must be guarded so in order to protect the full body from possible further harm. As it turns out, though, this muscle guarding is more likely to cause further potential harm than that which the body is aiming to prevent by muscle guarding.

At its core, muscle guarding is an effort by the body to defend itself against a perceived threat (whether remembered, anticipated, or actually present). But when no threat is present and the muscle guarding persists, then the behavior has the opposite effect, promoting more problems than it aims to resolve.
The Elimination of Protective Muscle Guarding with the X10 Machine
After completion of three weeks on the X10 Knee Machine (by week 12 post surgery), including three 30-minute sessions per day utilizing 7 lbs. of pressure modulation, Luis was able to achieve the following:
- Left Knee (Seated) AROM/PROM
- Flexion: 98º/114º
- Greatly improved gait pattern with no crutches (pain-free)
Luis began using the X10 Knee Therapy Machine in his home 3x per day, 30 minute duration for each session. His quest to avoid PT pain began in earnest. He found that because the X10 machine was under his control, he trusted that it would not hurt him. His brain (both subconscious and conscious) accepted this fact and he was able to relax during therapy. This allowed for real progress to begin again toward his range of motion goal of 130º. In three weeks Luis was able to gain 39º range of motion. He began walking as many as seven miles with less and less of a limp, at first using only one cane (vs. two previously) and then cane free.
The reactions at both Luis’ PT clinic and at his surgeon’s practice (Dr. Deepan Patel) were very positive. Luis was able to avoid a Manipulation Under Anesthesia as his range of motion exceeded the lower limits his surgeon set for MUA. Luis was able to overcome guarding, avoid PT pain, and get back on the path to recovery.
Through the use of the repetitive motion on the X10 Knee machine, motion that is controlled fully by the patient, Luis. was able to achieve relaxation “as control improved.” It was only after Luis “trusted” that the X10 Machine would follow his direction, never move past comfortable range of motion, only advance degree by degree as his leg became relaxed could avoid PT pain, that he began making significant gains. He overcame the guarding which led him to an ultimately successful rehabilitation.
In Conclusion
Source Material To learn more about Protective Muscle Spasms from Dr. Erik Dalton, Phd click Dr. Erik Dalton to visit his website. https://www.rennwellness.com/chiropractic/what-is-muscle-guarding.html https://cathedralchiropractic.com/2018/05/what-is-muscle-guarding/ https://www.novaactiverehab.com/pain-cycle/










Thanks for the share, rich article as always,
Maybe this could help for people who suffer from any muscles pain:
I am very against using any medicines or natural substances as there are a lot of dangerous things on the market these days. I saw a medicine on the doctors tv program and they had 3 women test it and all three had good results with no side effects. I bought it and hesitated to use it, however, I really hurt my back today and after resting, applying cold and heat and an Epsom salts bath, all of which didn’t help, I very lightly applied this to my lower back and immediately could feel relief. It feels a bit tingly but not burning at all, more cool. I won’t be without this anymore. Better than buying 10 products with minimal relief and no scary ingredients.For those who wonder where to get it, here is the official website and i think they still offer discounts:
mindbodymatrix.review-more.info