Podcast: Play in new window | Download (Duration: 33:52 — 77.5MB)
Subscribe: Apple Podcasts | Spotify | TuneIn | RSS | More
A Knee Recovery Nightmare!
Right Total Knee Replacement
My Physical and Emotional Fight Against Pain Hypersensitivity and Protective Muscle Guarding
– written by Cathy Banovac
– interview by Lisa Pelley and Mary Elliott
– Cathy was coached by Erin Rempher, PTA
My name is Cathy and I reside in Arizona.
I am 57 years old, a homemaker, and have had a genetic history of chronic osteoarthritis. From a very young age, I have always had a very low pain threshold. Prior to the commencement of pain in my knee, I considered myself a fairly fit and active person…loved gardening, entertaining family and friends, cooking, crafting, playing golf, traveling with my husband, walking our dogs, and playing with our grandchildren.
Life was good!

Early Summer
In addition to the normal aches and pains that come with aging, I began to experience more than usual pain in my right knee. I was experiencing daily occurrences of popping/clicking, giving out when walking at times, difficulty negotiating steps or stairs, and nightly interrupted sleep due to pain. Over the counter medications, icing, heat, etc. was no longer managing my symptoms. Upon visiting an orthopedic surgeon for examination and subsequent imaging, I learned I was over 70% bone on bone in my right knee joint. I was told I was looking at a total knee replacement. I was preparing to head to Michigan for a family vacation on the lake with my kiddos in August, so was not happy to hear this news. I convinced my doctor to give me a steroid injection just to buy me the time I needed to take my vacation. He was reluctant and told me that he predicted it would do nothing to help my condition at the very least or, at the very most, last for a brief time. I made it through the trip, yet 3 weeks post-injection the symptoms had returned.
No More Injections
My surgeon declined my request for another injection, instead reiterating my need for the TKR. Over previous years, I had witnessed my mother, father, husband and a few friends have knee replacement surgeries. All came through their surgeries with what appeared to me to be a fairly pain controlled, timely recovery and successful return to their regular daily activities. I was told I was on the younger side for this type of procedure, nevertheless, would greatly benefit from extended quality of life and return to desired activity, given my current quality of life and daily activity was becoming more diminished by the day.
My Knee Replacement
I underwent RTKR on September 25. All went well and as expected with the surgery. I was up and walking, began some light physical therapy exercises, and maintained post-op range and motion through use of a CPM while in hospital. I was discharged to home on the third day post-op, with a couple of narcotic pain medications (initially Percocet/Oxycodone and Morphine) and directions to commence in-home physical therapy the following day. My follow-up visit with the surgeon was scheduled for 6 weeks post-op. Day one at home began my challenging journey of recovery, both physically and emotionally. I experienced difficulty managing my pain even with narcotics and over the counter medications. My swelling was as expected and able to be kept in check with anti-inflammatory meds and icing. I experienced annoying side effects from the narcotics, i.e., headaches, nausea, constipation, and thus was bounced from one medication and dosage to another, none of which seemed to be the right combination or solution to my pain. Out of complete desperation and in uncontrollable pain, I went to the emergency room after being home for four days post-op, hoping to get some relief.
A Problem with the Surgery?
I thought surely there must be something wrong. A few hours later, together with a lecture from the hospital PT and some morphine, I was discharged back to home. Back on more medication, I failed to again find relief from pain. I was averaging about 2-3 hours of sleep per night and little sleep during the day. My home physical therapist had her work cut out for her. Over the next 4 weeks (twelve 45 min. sessions of in-home PT), I had yet to reach better than 85 degrees flexion and 10 degrees extension. My in-home therapist said she spent most of those 4 weeks strengthening my calves, hamstrings, and quad muscles, all which were extremely weak. Therefore, already I was approximately 4 weeks behind in range and motion advancement. My pain was still very much out of control, all while I feared becoming more and more dependent on the narcotics prescribed.
At the first follow-up appointment (six weeks post-op), my flexion was below 90 degrees and extension still not at the zero degree mark. I was informed by my surgeon that I needed a Manipulation Under Anesthesia (MUA). My knee felt very stiff, pain was still unmanageable, and I was stuck without advancement in physical therapy.

Manipulation Under Anesthesia
He took x-rays and made sure the appliance was not loose or slipping out of placement. All was found to be in proper order and an examination found no infection that could be causing pain or other symptoms. My surgeon had done his job. I was told however, that he believed I was stuck due to scar tissue build-up and thus was in need of the MUA to break up the scar tissue. This would also permit the ability to continue physical therapy, working towards achievement of the desirable degree of range and motion outcomes. I underwent the MUA six weeks and one day post-op and immediately resumed PT the following day. I was told not to worry about a reduction in my flexion and extension after having the MUA. An MUA tends to put patients back about 3-4 weeks, so it is almost like starting all over again. However, the idea is that advancement in range and motion should become easier now that the scar tissue has been broken up by the procedure. I went to PT for 5 days in a row the first week following the MUA, did my home exercises faithfully on my own twice a day, then returned to PT three times a week for the next several weeks.
After the MUA
At the two week follow-up appointment post the MUA, I was still in unmanageable pain, still getting only 2-3 hours of uninterrupted sleep per night, and running every gamut of emotion and temperament. My poor husband was beside himself and wondering whatever became of the woman he married 27 years ago. My flexion was still only reaching in the low 90’s and my extension was no better either. I was still experiencing great sensitivity to the touch anywhere on or around my surgical knee. I couldn’t stand wearing pants or having any sheet or blanket covering my knee. My pain was the worst at night, just when I was settling in for some restful moments on the couch watching TV with my husband. I would suddenly be lifted off my seat with either pain that mimicked touching a lit match to my knee, or the stabbing of a knife, or the shock of a taser.
Dealing with the Pain
This pain varied and sometimes was relentless for several minutes. I was in tears most evenings and headed to bed to ice or apply heat, which calmed the nerve pain somewhat. I would take meds (Hydrocodone/Norco, Extra-Strength Tylenol, Ibuprofen, Zofran (for nausea) Vitamins, a stool softener (due to Hydrocodone) and Gabapentin aka Neurontin. I was soooo sick of taking medications. I think my surgeon was beside himself as to how to control my pain and sensitivity, therefore, he recommended I seek help at a Pain Management Clinic for possible sympathetic blocks, as well as my medicinal pain management. Both he and my physical therapist told me I was forecasting pain neurologically before any exerted physical effort on their part was made to cause any pain. My intolerance for any amount of pain was prohibiting any measurable progress in my range and motion, thus scar tissue was building at a rapid pace. Physical therapy continued to be a challenge as I protective muscle guarded any force applied by my therapist to get better R&M. I cried through most of my sessions.
Pain Management
At my first appointment with the Pain Management Clinic, I met with the doctor. Most people have sympathetic blocks in their back to relieve nerve pain, but the doctor I was referred to chose to recommend a Genicular Neurotomy, accomplished through a procedure called Coolief Cooled Radiofrequency Ablation. I first underwent a test which involved Lidocaine injections in four areas surrounding my new knee. The patient then logs their pain and activities over the following 72 hours. A follow-up appointment with a Nurse Practitioner then reviews the log and determines eligibility for the ablation procedure. At this appointment she chose to cut my medication cold-turkey for a couple of days as she deemed I was dependent on them, even though I was getting little pain control. I experienced severe withdrawal symptoms for two days.
A Change in Medication
I thought I was going to go out of my mind. A change in my medication increased the Gabapentin I was taking, and I was found to be eligible for the ablation. I underwent that procedure approximately 6 weeks post my first MUA, just before the Thanksgiving holiday. I was told that I would still be experiencing pain for approximately 4-6 weeks, due to the fact that the ablation was going to make my nerves “angry” as they fought their temporary death. I was also informed that this procedure is temporary as nerve endings most often regenerate themselves over a 6 month to 2 year period. Some patients must undergo two or three of these procedures to get lasting relief.
Unhappy News
This was not happy news to my ears, yet I was still desperate for relief and reaching out for anything, and I mean anything, that would control my pain. I returned to the pain clinic for a follow-up to the ablation procedure only to report pain still very bad and that I was still taking a boatload of medication, icing, heat to quad muscles to relieve cramping, and poor results in physical therapy sessions. I was told to give it more time and come back in a few more weeks. At my next follow-up approximately 3 weeks later, I discharged myself from the Pain Management Clinic. I felt that their treatment plan was not successful for me and they had no other plan to offer other than continued reliance on prescription medication and time.
When recovery goes wrong – Read More
A Desparate Time
After barely getting through the Christmas holidays, persisting in physical therapy and weaning myself down on prescription medications (since they didn’t seem to be having any great effect on my pain), I began to explore the possibility of medical marijuana as a solution to my pain control. I have never tried marijuana and had little desire to smoke or vape it, but was interested in edibles they have out now. I was desperate and finding myself sinking into anxiety, panic attacks and, at times, depression. My family and my husband were becoming very concerned as I was changing into a person they did not know and they were at a loss as how to help me through my circumstances.
Medical Marijuana
Since medical marijuana is legal in the State of Arizona, I sought out a doctor with whom I met and applied for a patient card. This process took approximately 3 weeks, including approval of my application through the Arizona Department of Health and Human Services. Upon receiving my card, I met with a licensed nurse at a dispensary to become educated about the various products and my specific needs. She was recommended by the doctor who signed off on my patient eligibility and works with a number of cancer patients to help control their symptoms. We met for over an hour. She was extremely patient with me, educating me about cannabis (which I knew little of) and gave me recommendations to try. I purchased three of her recommendations. I also decided to try getting a light massage once per week. The massages lasted for approximately three weeks before I decided to suspend them, as I found them not helpful enough to warrant the expense.
Little if Any Improvement
Having done everything I was asked to do in my recovery and still making little if any gains, I found myself in a very dark place emotionally, desperate to end my pain, and I was done!! One day, I was occupying my time, in between home therapy and out-patient therapy sessions, searching the Internet for anything that might literally save me. When in answer to my prayer, I came across several website postings about a therapy called X10. I shared some of it with my husband, my parents and my kids. They encouraged me to explore it more. After reading some of the patient blogs and watching a few of the videos that I could access, I made my first contact with PJ Ewing by emailing him. PJ responded very quickly telling me that the X10 Therapy and machine was not yet available in the State of Arizona, but he provided me with some other resources. I was initially devastated by this news, but I almost immediately decided that I was not going to accept that response. I instantly thought to myself, “Well, if it is not available in AZ, then maybe I can travel to wherever it is available.
Not Taking ‘No’ for an Answer
This time, I placed a phone call to PJ and we talked for over an hour. As it so happened, in our conversation I discovered that the X10 headquarters is in Franklin, MI, and I had family who lived in Rochester, MI. PJ was more than gracious in discussing all the parameters and specifics of the possibility of travel to Michigan to undergo the X10 program. To say the least, after completion of my discussion with PJ, I heard God say “Not yet, Cathy, I still have a plan for you on this earth.” I discussed the possibilities with my husband and shared them also with my son and daughter-in-law, exploring their permission to have me as a houseguest for 2-3 weeks. Of course, they couldn’t have been more gracious and welcoming.
Pain Still a Big Problem
My pain was still out of control, I continued out patient PT three times a week with slow or little advancement in my R&M, had my six week MUA follow-up with my surgeon only to be told I was facing a second MUA. I told my surgeon and my physical therapist about the X10 Therapy website I had discovered, and PJ sent me the clinical data to share with them. Each of them, I am grateful to say, told me they had looked at the data and were “intrigued” by the therapy plan. Both encouraged me to pursue it as an option for me, yet both also strongly indicated that enough time had passed between my first MUA and the ablation, therefore, still recommended I have the second MUA before commencing X10 Therapy.
Turning to X10 Therapy after a Second MUA
Once my husband and I had made the decision to pursue this plan, the wheels began to roll quickly. Initially, I scheduled the 2nd MUA and a flight out from Phoenix to Detroit by myself the next day following the MUA. I notified PJ of my plans and he began to put things in motion by placing me in contact with Mary Elliott, Melissa, Mike, a therapy Coach, Erin a Physical Therapist, and Marty, a technician for machine home delivery and set-up. The X10 Therapy approach is really a “team” approach to wellness, in addition to the machine itself and the technological programs it delivers to the patient.
The Second MUA Was Coming Up
As the days approached the 2nd MUA, I became extremely anxious and experienced a couple of panic attacks. I began to stress about the MUA pain, having gone through one already. The thought of flying alone, even though my son would be there to meet me at the other end of my flight, and having to get through a 4 hour flight plus 1 hour car ride to his home in pain, had me scared beyond belief. I was consumed with thinking about how I would manage my pain. Should I just knock myself out to sleep on the plane? What if that didn’t work? What meds could I then take if in pain? What about my leg position – straightening and bending? How would I get help from curb, through security, to gate, onto plane and the same again when arriving including a stop at baggage claim? How am I going to sleep at night? Is this therapy going to put me back in unmanageable pain again, even though the X10 Therapy information says I am in control? What if it doesn’t work? Can this end my knee recovery nightmare? And on and on and on…!
Making Plans
After talking it over with my husband and doctor, it was decided that I would delay my trip to Michigan for one week following the 2nd MUA. I would continue outpatient PT immediately following the MUA, but have some time to consult with a psychologist concerning my sleep depravation, fears, anxiety/depression and develop a plan to manage my pain, as well as talk to the airline for special assistance to help solve my transportation needs. My husband decided to make the trip with me for a couple of days, just to get me settled and started with X10 Therapy. Armed with a revised medication and travel plan, I notified the X10 Team of my change in start date and all were extremely understanding and accommodating. I had the 2nd MUA on January 18. I continued outpatient PT for three more sessions, in addition to my own home exercises twice per day. My daily sleep and pain control was managed better and I was counting the days until our departure date. It simply could not arrive fast enough!




Friday, January 19
This will remain a very important and pivotable day in my life. My journey towards healing, life anew and well-being would begin that very day. Having endured a comfortable flight and having managed all the transportation arrangements with ease (kudos to Delta Airlines), we arrived at my son’s home ready to commence what I can now claim as my own personal miracle. Within an hour, Marty arrived with a smile, this technological marvel known as the X10 machine, and a thorough first orientation/training session filled with words of encouragement and confidence. I was on my way, although until I began to see results (which were really displayed within that first session),
I Had Hope
I was still cautiously optimistic about where I was headed. Could I really achieve the flexion and extension goals I was unable to achieve thus far with any of my existing recovery methods? Would this therapy really enable me to manage my pain comfortably with mild medications? Could I trust my X10 therapist and her plan for me? Would the X10 team really be there for me when I needed them? Was the X10 therapy the answer to my prayers? Would I really be returning home in as little as just over 2 weeks time to see my surgeon’s and physical therapist’s jaws drop as they witnessed my flexion and extension reach what we all thought would be skeptical results, but instead blow them away with incredible success? It would not be long before I could actually acknowledge to myself that the answers to each of those questions would be a resounding YES!
110º Flexion
Once I was able to reach the 110 degree mark for flexion, it was decided that I would add 5 min a day on the stationery bike. As I felt comfortable, I was able to increase that time in small increments and add another bike session in the evening. While my progress was measurable daily, I did experience some cramping in my right thigh and calf, dealt with some bursitis in my right hip for about two weeks, and waking with some right leg pain some nights.

Taking Care of Myself
I found icing and elevating regularly after each exercise session, icing my hip, heat on my upper thigh at night, Tramadol 50 mg. only twice a day with Ibuprofen and Acetaminophen alternated during the day, and Theraworx Relief foam massaged in the cramping areas once or twice a day helped keep my discomfort manageable. In addition, I spent some resting time researching dietary recommendations for inflammation and pain. I incorporated tumeric, magnesium, Osteo Bi-flex, 100% Cherry or Pineapple Juice, Vitamin B6 & B12, Vitamin C, Vitamin D3, Zinc, fresh berries and decaffeinated tea with ginger, lemon and honey in my daily diet. I also decided to limit carbohydrates and sugar intake in an effort to keep my inflammatory response in check.
One Week In
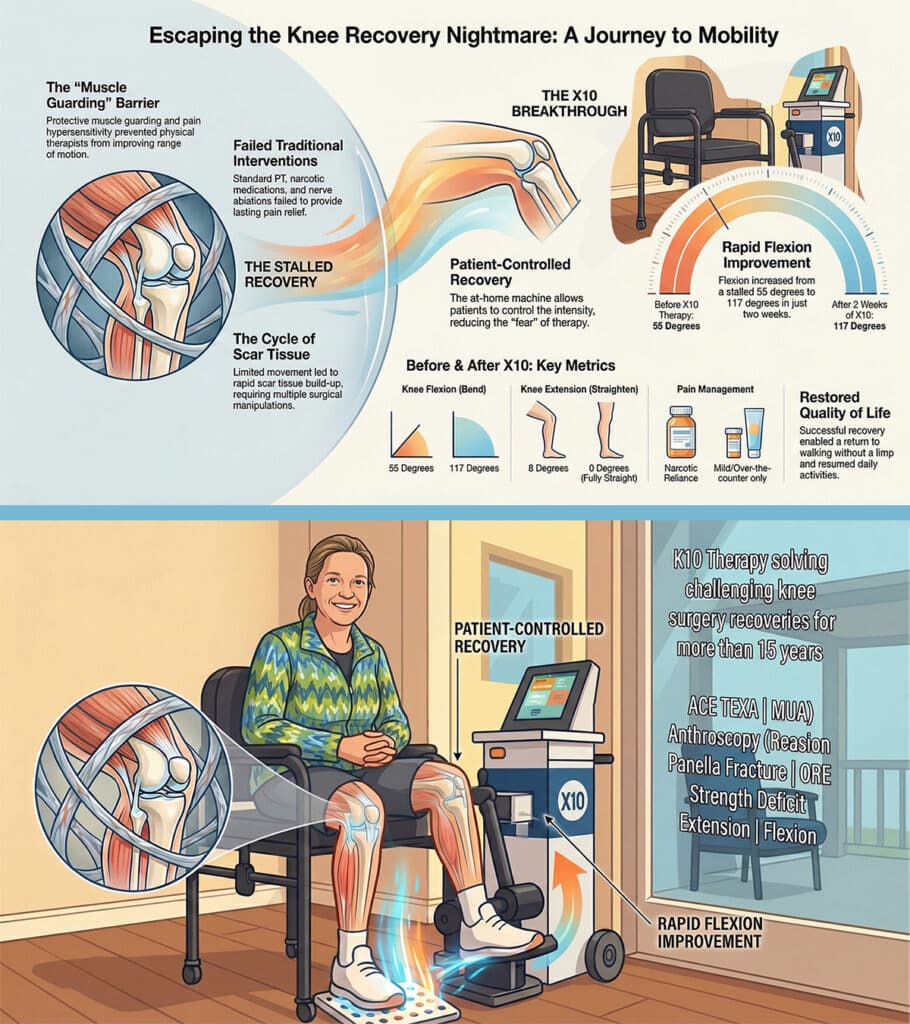
After one week on the X10 and with constant reassurance and communication from all of my X10 team, I could actually begin to call this journey and the X10 Therapy my miracle. I had breached the 100’s for flexion after starting at 55 degrees, and reached 0 degrees at the end of the first session on my extension, previously at 8 degrees. My fears, anxiety and uncertainty soon gave way to renewed love for life, joy at gaining confidence in doing daily activities again, sharing my daily success by telephone with family and friends, and hope for the future. The almost daily contact from one or more of my X10 team members answered any questions that arose, provided authentic cheerleading for my cause, and motivated me to press on for better and better results.
Working with My Coach
Mary called often to check in with me and was my calm and steady encourager. My conversations with her were uplifting and kind of like talking to an old friend, casual and comforting. My PT, Erin, made a home visit to discuss my history and offered varied strategies for increasing my flexion degrees, as well as made adjustments in my therapy plan due to some bursitis that I had recently developed in my right hip. She was careful to make the appropriate adjustments to my therapy plan. She and Mike (my strengthening coach and with whom I also met in person to go over exercises), together modified my plan by delaying some of the exercises, while still permitting three sessions a day for range and motion growth.
Conclusions
As I approach my last day of sessions on the X10 Therapy machine and a return home to Arizona tomorrow, I write my story to encourage anyone who has experienced one or more of the circumstances that I experienced subsequent to a total knee replacement. I am happy to report that I was successful in breaking through some of my scar tissue, reaching 0 degrees for my extension and 117 degrees flexion. My gait is much improved and, as I have returned to walking without a limp or dragging my surgical leg, the pain in my hip and lower back has also improved greatly.
My knee recovery nightmare has finally come to an end.

Some Rehab Insurance
I will continue outpatient therapy immediately upon my return home in order to solidify my current range and motion, and even further improve my flexion as I am able. I write this also as a means of paying it forward to future patients of the X10 and in grateful appreciation to my X10 Team, my family and my friends who affirmed, guided, encouraged, and yes, celebrated, my X10 Therapy journey of success. The proof, as they say, is in the pudding, which is said to mean that you can only judge the quality of something after you have tried, used, or experienced it. I absolutely cannot wait to share my experience and demonstrate my range and motion achievement in person to my surgeon and PT Team back home in Arizona.
Thanks be to my God, to all of my support team and to X10 Therapy…
life is good once again!
To read about total knee replacement for a younger population, click here.
The X10 Meta-Blog
We call it a “Meta-Blog” because we step back and give you a broad perspective on all aspects of knee health, surgery and recovery.
In this one-of-a-kind blog we gather together great thinkers, doers, writers related to Knee Surgery, Recovery, Preparation, Care, Success and Failure. Meet physical therapists, coaches, surgeons, patients, and as many smart people as we can gather to create useful articles for you. Whether you have a surgery upcoming, in the rear-view mirror, or just want to take care of your knees to avoid surgery, you should find some value here.











WOW! What a story Cathy. I am so happy to read that you have regained the ability to enjoy life again!! Congratulations on your results and on the fact that you did not give up when it seemed like there was no solution available out there to help you out with your knee flexion and pain management. The X10 is an incredible machine and your story is once again the proof that it can do amazing things. Wishing you all the best for the future, living an active life with your loved ones.
Cathy!
You put your story into words with grace, strength, and bravery – just like you faced your recovery with the X10! I am so proud of the progress you made with us and am blessed to have been a part of the process! I will direct others to read your story and find that there is hope, even when there are challenges, following a knee replacement. Best wishes always,
Erin, Patient Recovery Coach & PTA
Cathy we have been so pleased to meet you and work with you on your knee recovery! Truly you have made such an impression on everyone in our company!!
….I have been a subscriber to the seemingly fabulous X10 blog since prior to my own TKR in January 2017 which appeared to go well from a surgical standpoint – for me minimal pain and even when I returned home on the 4th day post surgery and had to get up the 22 stairs leading to my upper duplex, there was no issue. (even with my DVT).
However, the issues started when in our poor health care system which used to provide a good 2-3 weeks of being in a rehabilitation facility and having physio 2x a day – we only receive a 1/2 hour home visit, 2X a week from a physiotherapist, who is more intent on reaching the guideline specifications of his schedule and where a knee should be bending after so many days, weeks, etc, that he forced the knee each and every time to bend, which did nothing more than cause great amounts of pain, followed by days of recovery and an instinctive resistance each time he would return thereafter. I finally had to hire a private physiotherapist, in tandem, who would visit 2-3X a week with a different approach.
However, the arthrofibrotic tissue (scar) had already settled around my knee and it wouldn’t even make it to a 90 degree mark.
I would have done anything to get the X10 (my orthopedic surgeon didn’t quite believe in it…but for some reason, all my reading turned into some “religion” whereby I totally believed it was a machine that would have answered all my problems. Unfortunately, in Canada, we don’t have them.
I had the manipulation within 2 months of the surgery….but again, the scar tissue beat us before my knee would bend to the proper degree. It is now 14 months later and I purchased a commercial style exercise bike (would have preferred the Pilates reformer or Cadillac but the prices were exorbitant) to try and get the knee moving. The thing is, a knee can’t do a bike unless it can bend at 110 degrees….so, I have to hike the seat up so high to at least get the momentum…(which of course forces the opposite hip to jut out and then causes lower back strain)…
My 2nd knee requires the surgery but the orthopedist won’t touch it until the first one is working properly. He has suggested another manipulation – or perhaps arthroscopic surgery to remove the scar tissue. But for me both choices lack logic as my body has proven to produce an excessive amount of scar tissue which no doubt will return again once the site has been “injured”…
I think the X10 is amazing…and that is only from afar…
Cathy you are lucky…and it is so wonderful to hear a story with a great ending…! I am so glad you persevered…
LG
Such an interesting story. I could if written it myself word for word. I had both knees done at once. I’m about to have my second manipulation. I was tested for the ablation, but opted out. My ROM after 4 months is -5 on extension and 90-94 flex. I’m at a very low point. My question is, how are you doing with your knee today?