Recovering from Knee Replacement Surgery: What you rarely hear, and how to prepare for it
By Dr. Carl Freeman (Professor of Biology at Wayne State University)

MRI Knee Replacement
Knee replacement surgery is extremely effective at eliminating osteoarthritic pain. But, recent research shows that, “Current practice of total knee replacement as performed in a recent U.S. cohort of patients with knee osteoarthritis had minimal effects on quality of life and QALYs (quality adjusted life years) at the group level.”
I believe that a major reason quality of life is not significantly enhanced by knee replacement is because of standard physical therapy, which on average, results in a 50% strength reduction at one month post-surgery, and a 30% strength deficit for one to 13 years after surgery.
What is commonly discussed among surgeons and physical therapists is range of motion, which encompasses both your ability to straighten your leg (extension) and bend your leg (flexion). You need to be able to straighten your leg, and bend your leg to about 110-115 degrees. Unless, you achieve these benchmarks, you won’t be able to engage in many activities of daily living (ADLs). You must regain an adequate range of motion—if you don’t your surgeon will likely perform either a manipulation under anesthesia or a second surgery called an arthrolysis. The latter is used when scar tissue formation is extensive—usually more than 2 months after surgery. Either procedure causes you to start your rehabilitation over again. So, therapists work extremely hard to gain range of motion. But, having achieved a range of motion that should allow you to engage, say ski, does not mean you have the strength to go skiing. It merely means you can adequately bend your leg.
Let me explain how these consequences arise and how a simple to use, new, invention can resolve both the range of motion and strength issues within a month—but it’s so new your surgeon may not know about it yet. You can share what you learn here and refer your surgeon to x10therapy.com.
Causes of Strength and Range of Motion Problems
Your body cannot tell the difference between surgery and trauma—and responds to surgery exactly as it would if your body had experienced traumatic injury. Consequently, your body sends inflammatory cells to the site of injury to help heal it, and the damaged cells and blood vessels leak fluid —creating swelling in, and around, your knee.
What patients are rarely told is how bad this fluid is. Your body interprets pressure, caused by swelling as pain. And, a mere 30 cc of fluid can totally prevent you from bending your knee; this fluid also inhibits your voluntary muscle control of your legs, and finally, the fluid contains chemicals that promote scar tissue formation.
The single most important thing you can do is to pump the fluid out of your leg (into the lymph—then to the blood, and finally out of the body in the urine). Pumping requires that you bend your knee and flex your leg muscles—which, as I have just discussed, is difficult. Because you cannot do this effectively, someone else, usually your physical therapist (in standard therapy) will bend your leg for you. To do this they usually push or pull on your leg, to bend it, as far as you can stand it; for as long as you can stand it. This bending really hurts– because it adds pressure to an already swollen joint. Therapists typically repeat this pumping process three to five times at each physical therapy visit— (three times a week). Sometimes, they push too hard and damage your knee causing more swelling and pain. In other cases, they don’t push hard enough and little fluid is pumped out of your knee.
Hand-pumping typically results in a few degrees gain in the range of motion in a week or two—or longer. Not only is it ineffective, but because hand-pumping hurts, many patients do not attend all their physical therapy sessions (noncompliance) which cause the swelling to persist making the problems worse.

Physiotherapist Knee Mobilization
Interestingly, studies show that therapists are remarkably consistent in how hard they push– which is another way of saying that they have real trouble adjusting how hard they push to the patients’ needs. Therapists cannot recalibrate their arm. But as we will discuss below—computer controlled arms are infinitely adjustable and ironically provide better individualized care than a human physical therapist.
For many knee replacement surgery patients, these knee problems come as a surprise, because in the hospital, they had physical therapy and could readily bend and straighten their leg. But, as the regional pain block wears off, your range of motion can decrease by 30-50 degrees or more, and you will probably not be able to straighten your leg either.
Surgery is the first half of process to deal with knee osteoarthritis, and it was easy—you slept right through it. Recovery is the second half and it is up to you and your physical therapist—you can do it the old-fashioned way which is slow, painful, and hard. Or you can use a new machine that makes it fast, easy and nearly pain free.

The most complete knee recovery system ever created — Read More
Physical therapy, as a discipline, dates to WWI, and the essential feature for gaining knee range of motion—is the painful, ineffective, hand pumping which has not changed in the past century.
The consequences of not getting the fluid out quickly are:
- prolonged pain
- scar tissue formation and perhaps a painful manipulation or additional surgery required to break it; 3) a strength deficit and muscle atrophy because the fluid has prevented voluntary muscle control (via neural muscular re-education) so you could not exercise your leg muscles.
Following knee replacement surgery, you are in pain, and the last thing you want to hear is how urgent it is that you get rid of the fluid—which will increase your range of motion and mitigate the adverse consequences discussed above. But, the truth is that you are in a race to gain range of motion and break up the scar tissue before it forms fibers. Once fibers have formed you can no longer increase the flexibility of joint beyond what it has– without medical intervention.
Thanks to a modern invention in the X10, you no longer need to experience the pain of having the therapist push on your leg. The fluid can be removed so fast that your needing a manipulation or follow-surgery is extremely unlikely. Finally, the faster the fluid is removed, the less of a strength deficit you will experience — and the shorter the time you will have this strength deficit.
Consider the following data from the X10 Knee Recovery System™
Fifty percent of patients have achieved 90° in six days. At 90° range of motion you are no longer at risk of having a manipulation. By 12 days over 75% are out of danger and by 17 days 90% are at 90°or beyond. In standard physical therapy results like these take several months.
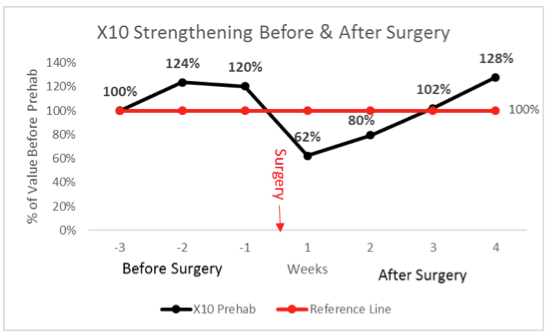
Now let’s look at strength. One of the things we at X10 Therapy advocate is pre-surgical strengthening.
The above graph looks at patient strength about three weeks before knee replacement surgery and then again about the day before surgery. All these patients used the X10 for strengthening. I am only showing strength for the quadriceps muscles, the main muscles doctors worry about (but similar results for all leg muscles groups have been observed). I divided the patient quadriceps strength before surgery by what it was when they started using the machine for exercising. The red line indicates no improvement. What we see is that all the patients became stronger, some by 7% others by 14-16% and one patient gained 55% over their baseline value. So, pre-surgical strengthening on the X10, done in your own home, yields results comparable to eight weeks of exercising at physical therapy clinic. The X10 had 100% compliance, whereas the physical therapy clinic had only 42% compliance.
What really matters is what happened after knee replacement surgery.
After knee replacement surgery, the same patients used the X10 for strengthening. Instead of a 50% strength deficit at 30 days, (which is what standard therapy yields) we see that our patients have regained 90% of their strength or more. Some knee replacement surgery patients are actually stronger than they were before surgery.
This is unheard of with standard therapy.












I am aware of the X-10 capabilities. I am deciding on surgery in December, but live in San Jose, CA. Last I checked this machine was only available in very limited, select locations in Florida and upper mid-west. I would like to know exactly where it is currently available. Perhaps I can find a location near a friend or relative, or maybe rent a motel room for a week or two during recovery.
My knee was successfully replaced last November and I am happy with the knee, but my range of motion is less than I would like. The Doctor can re-open the incision and do an extreme articulation of the knee before re-closing. Then the range of motion can be exercised once again during this second healing period with the possibility of increasing the range. That is my goal.
Richard
Richard:
We are as of yet not in California. A link to our geography is here… but I bet you have seen that already:
https://x10therapy.com/availability/
We are expanding. That is the good news!! Expect more growth geographically within the next 6 months for sure.
PJ
Basically, with the help of X10™, a knee surgery operation patient can regain around 90% of their strength or more within 30 days against the mere 50% before as you’ve mentioned. That is extremely jaw-dropping as it’s a real innovation when it comes to knee surgery. They should be able to live a normal life quite soon after the operation as this expedites their recovery time way faster than before. I’ll try to read more about the current practices in knee surgery before having my dad operated. He’ll surely be happy to hear that he’ll be able to use his legs properly again soon. Thanks!
It’s great to learn more about knee surgery. I never thought about how the body reacts to surgery like it does to trauma. Now it makes sense why surgery has such a long recovery time!
My grandfather has knee problems and he’s having a hard time sleeping lately. It was mentioned here that having a knee surgery is effective to eliminate knee pain. Furthermore, it’s advisable to consult professionals for a knee surgery.
Hi Dr. Carl, thanks for helping me understand that there are two phases that we need to consider in having a knee replacement surgery. First, is the surgery itself, and second, is its recovery. Just in case my dad will undergo in this procedure, I will see to it that we’re all here to support him. Cheers!
Thank you for the post on what I need to know about a knee replacement. I definitely think if no amount of medication or physical therapy is helping with the pain or ease of use anymore then it might be time to consider knee replacement surgery. You don’t want to be in pain every day and you want to get back on your feet and enjoying your life.
My grandmother is having a hard time walking because of her knee and she’s considering knee replacement. It was explained here that when recovering from knee replacement, she needs to be disciplined. Furthermore, it’s recommended to go to trusted health professionals for quality knee replacement.